AI Benefits Enrollment
Enroll Benefits. Zero Manual Work.
Use StackOne to connect your AI agent to your HRIS, benefits administration, and payroll systems to automate benefits enrollment.
AI Agents
Connect
MCP and A2A to REST, SOAP, and proprietary APIs.
Optimize
Tool discovery, data shaping, and reliable execution.
Secure
Scoped permissions, audit trails, and observability.
StackOne Integration Layer
Connect
200+ connectors, build your own, and multi-protocol support.
Optimize
Context, token, and speed optimization infrastructure.
Secure
Permissions API and prompt injection protection.
What Can AI Agents Do for Benefits Enrollment?
Your agent handles the full enrollment pipeline — from detecting life events to confirming elections — pulling eligibility data along the way.
Validate Eligibility
Pull employee profile, employment status, and plan eligibility rules from the HRIS. Apply logic to determine which benefit plans the employee qualifies for based on role, tenure, and employment type.
Collect Elections
Guide the employee through plan selection, coverage tiers, and dependent management. Validate and store supporting documents for qualifying life events via Google Drive or SharePoint.
Submit to Carrier
Transform election data into carrier-specific formats and push to benefits administration platforms. Use Connector Studio to build custom integrations for carriers with proprietary APIs.
Detect Enrollment Triggers
Monitor open enrollment windows and qualifying life events — marriage, birth, job change — from Workday, BambooHR, or Rippling.
Validate Eligibility
Pull employee profile, employment status, and plan eligibility rules from the HRIS. Apply logic to determine which benefit plans the employee qualifies for based on role, tenure, and employment type.
Collect Elections
Guide the employee through plan selection, coverage tiers, and dependent management. Validate and store supporting documents for qualifying life events via Google Drive or SharePoint.
Submit to Carrier
Transform election data into carrier-specific formats and push to benefits administration platforms. Use Connector Studio to build custom integrations for carriers with proprietary APIs.
Why Building a Good Benefits Enrollment AI Agent Is Hard
Connecting to 20+ HRIS and Benefits Providers
An enrollment agent needs to read employee records from Workday, BambooHR, or ADP, check eligibility rules per plan, and write elections back. Building and maintaining connectors for each — SAML vs OAuth, SOAP endpoints, provider-specific rate limits — is a massive lift.
Token Cost Multiplies During Open Enrollment
Without search-first architecture, the agent pre-loads every HRIS and benefits action definition before processing a single election. During open enrollment, hundreds of employees hit the agent simultaneously — token costs spike across every tenant.
Benefits Data Carries Prompt Injection Risk
Enrollment agents process employee-submitted data — dependent names, life event descriptions, uploaded documents. A single adversarial string in a benefits form field can hijack the agent into approving ineligible elections or leaking plan details.
Getting High Accuracy Requires Purpose-Built Tools
Processing elections accurately requires reading employee eligibility, validating dependent relationships, and writing the correct plan selections back to the HRIS. Raw API wrappers expose too many low-level details and lead to hallucinated field values.
How StackOne Makes Benefits Enrollment AI Agents Possible
Everything your enrollment agent needs to read employee data, validate eligibility, and process elections — with the controls HR and IT demand.
200+ connectors with 10K+ agent-optimized actions
Pre-built connectors for Workday, BambooHR, ADP, Rippling, UKG, Gusto, and Personio with full native HRIS action coverage for benefits workflows.
Managed Auth handles credentials across providers
OAuth flows, API keys, and SOAP service accounts managed per tenant for every connected HRIS — no custom auth code for Workday, ADP, or Rippling.
Search and execute finds the right action
Agent searches StackOne's catalog by natural language and executes the matching HRIS or benefits action — no pre-loading thousands of tool definitions during enrollment surges.
Managed Webhooks deliver enrollment events consistently
StackOne normalizes enrollment triggers — open enrollment windows, life events, status changes — as reliable webhooks with synthetic polling fallback for providers lacking native events.
Connector Studio extends to carrier APIs
Build and deploy custom connectors to insurance carriers and benefits platforms with complex APIs using a YAML framework — ship new carrier support in hours, not months.
Defender blocks prompt injection from enrollment data
StackOne Defender screens employee-submitted fields — dependent names, life event descriptions, uploaded documents — for injection attempts before the agent processes them.
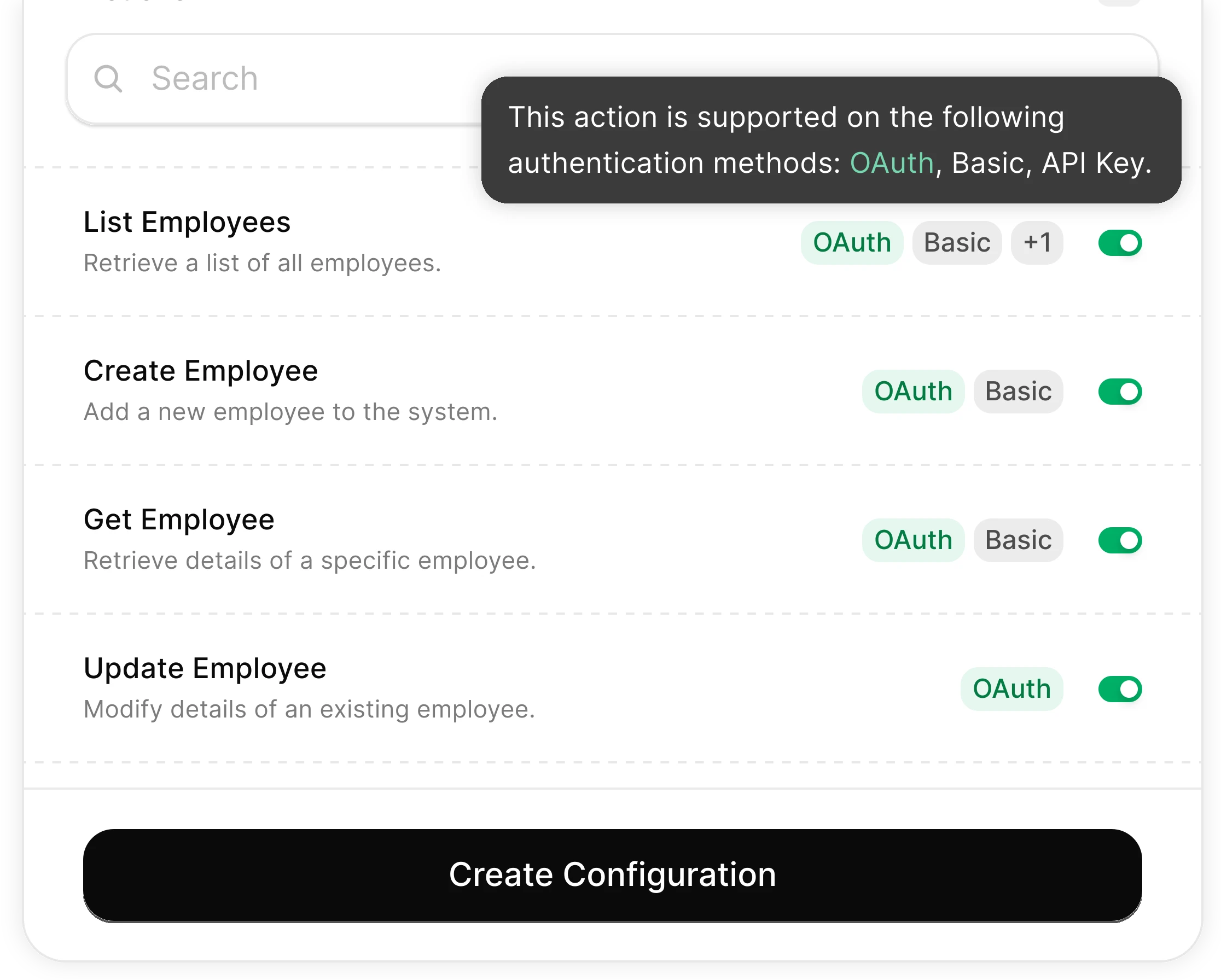
You Control What the Agent Can Do
Scoped permissions define exactly which employee data the agent reads and which benefits actions it takes. Full audit trail of every enrollment operation for HIPAA and ERISA compliance.
Connect Any Agent to Automate Benefits Enrollment
Any Agent Framework
Claude, OpenAI, LangChain, Vercel AI SDK, CrewAI, Pydantic AI — StackOne works with every major agent framework out of the box.
Any Agent Builder
Whether you're building with code, a visual builder, or an enterprise platform — StackOne provides the integration layer your agent needs.
Connect Your Agent to Your HR Stack
Start building in minutes. MCP connectors to every system your agent needs.
Frequently Asked Questions
Connect Your Agent to Your HR Stack
Start building in minutes. MCP connectors to every system your agent needs.